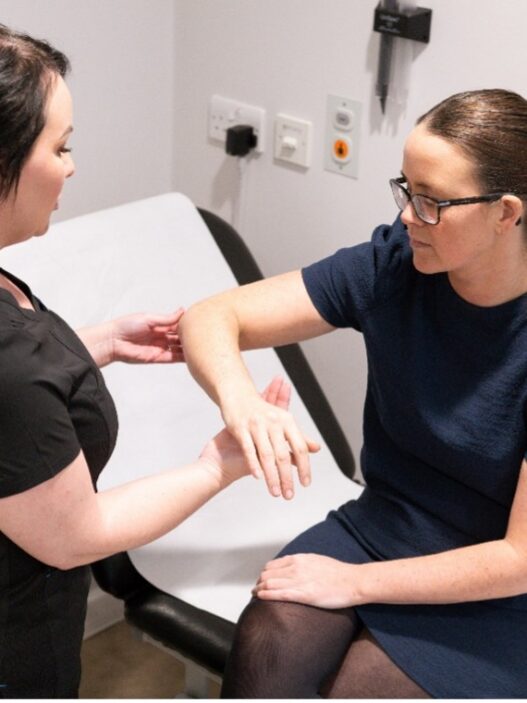
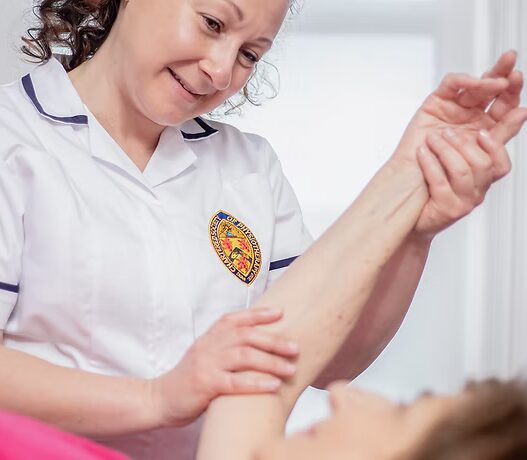
By Prudencia Lyons, from Rejuvenate Lymphatics Therapy
Lipoedema is finally gaining long overdue attention and for many women, that recognition matters. When public figures such as Josie Gibson speak openly about their diagnosis and treatment journey, it helps validate the experiences of countless women who have lived for years with pain, swelling and the feeling that their bodies were misunderstood. Her story reinforces a vital message: Lipoedema is about health, not weight or willpower.
But awareness must be handled responsibly. As media attention grows, so does the need for ethical, evidence-based care, particularly for women who may be newly diagnosed, vulnerable, or still seeking answers.
What Is Lipoedema and How Common Is It?
Lipoedema is a chronic disorder of fat tissue that almost exclusively affects women. It causes disproportionate fat build-up, most commonly in the hips, thighs and legs, and sometimes the arms, while the hands and feet are usually unaffected. The tissue can be painful or tender, bruise easily, and create a heavy, aching sensation. Crucially, this fat does not respond to diet or exercise in the usual way.
Although Lipoedema remains under diagnosed, research suggests it may affect up to 10–11% of women worldwide, with similar prevalence widely cited in the UK.¹ Despite this, many women spend years without a clear explanation for their symptoms.
Quality of Life: The Heart of the Conversation
For women living with Lipoedema, the impact goes far beyond appearance. Research consistently highlights significant effects on quality of life, including chronic pain, fatigue, reduced mobility and difficulty with everyday activities.² Many women also report emotional distress, social withdrawal and a loss of confidence not because of how they look, but because of how the condition affects how they live.
This is why recognising Lipoedema as a genuine health condition matters. Quality of life should sit at the centre of every conversation about diagnosis, treatment and long-term support.
Diagnosis: Why It Can Take Time and How to Navigate It
Lipoedema remains under-recognised in medical training, meaning women are often misdiagnosed or told their symptoms are simply weight-related. Securing a diagnosis can take time, but it is an important step in accessing appropriate care.
Keeping a clear record of symptoms such as pain, tenderness, bruising, disproportionate fat distribution and changes in mobility can help when speaking with a GP.
Referral to clinicians or services familiar with lymphatic and fat disorders may support more accurate assessment and informed care planning.
Emerging Evidence: The LIPLEG Study and International Dialogue
Recent international research is shaping the future of lipoedema care. The LIPLEG study, a large multi centre randomised clinical trial, compared surgical treatment (liposuction) with conservative management and demonstrated significant improvements in pain, mobility and quality of life for women undergoing surgery.³ Its findings were discussed at the Lipedema World Congress in Rome, highlighting growing global collaboration and scientific progress.
In Germany, this evidence has led to public health insurance funding liposuction as a medical treatment for Lipoedema a development that has prompted important conversations across Europe about access, ethics and evidence-based care.
NICE and the UK: What Are the Next Steps?
In the UK, NICE has previously called for further high-quality evidence before recommending surgical treatment for Lipoedema on the NHS.⁴ With the LIPLEG study now published and internationally recognised, the next steps are likely to involve continued evidence review, further research and ongoing advocacy centred on patient-reported outcomes and quality of life.
Progress will depend on collaboration between patients, clinicians, researchers and policymakers ensuring women’s lived experiences remain central to decision-making.
Finding Trusted and Ethical Care
As awareness grows, choosing ethical care becomes increasingly important. Practitioners whether therapists, GPs, or surgeons should be transparent, realistic, and patient-centred, focusing on supporting quality of life with realistic expectations.
Rejuvenate Lymphatics Therapy is one example, offering lipoedema-informed care grounded in ethics and evidence. Their team supports women through diagnosis, conservative management, and discussions about ethical surgical options, providing compassionate, patient-centred care focused on quality of life.
Trusted organisations such as Lipoedema UK and MLDUK (Manual Lymphatic Drainage UK) offer education, professional standards and guidance to help women navigate care safely and confidently.⁵
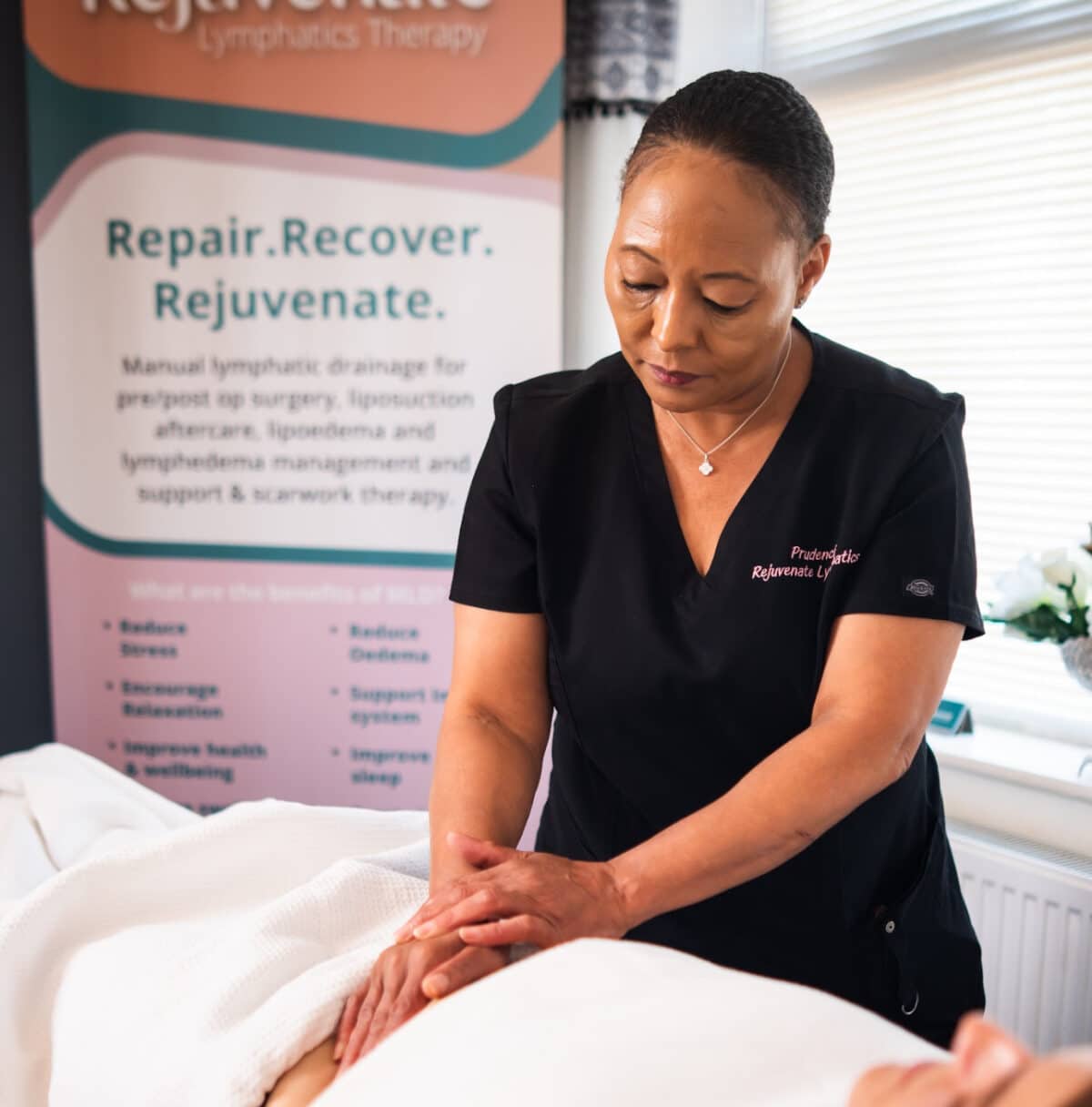
Rejuvenate Lymphatics Therapy
Prudencia Lyons
recovery care, and ScarWork therapy.
Prudencia Lyons has a deep and personal passion for raising awareness of Lipoedema, supporting clients with education, care, and treatment tailored to their unique needs. Every treatment is delivered with compassion, professionalism, and a results-driven approach.
Registered Nurse.
Certified Manual Lymphatic Drainage (MLD) Therapist –
(Vodder Trained (level 3).
Specialist training in Lipoedema & Lymphoedema management
Post-operative recovery care & ScarWork Therapy.
Advanced Diploma Blend Oncology Specific Training for Soft Tissue Therapists
Contact Rejuvenate Lymphatics here.